Marathon season is now upon us. Runners of every level have been training throughout the summer months for their fall races. Whether you’re a seasoned runner or just starting out, you can get overuse injuries during the last push of training before the big race. Douglas Solway, DPM, podiatric surgeon at Illinois Bone & Joint Institute (IBJI), discusses common foot conditions and pre-dislocation syndrome (PDS) that can arise from training.
Solway says that some common foot conditions that could result from training include plantar fasciitis, Achilles tendonitis, shin splints, nail hematoma, and stress fractures; all of which are usually fairly straightforward in terms of diagnosis and treatment. Some runners are not familiar with PDS, the condition that is based more on your anatomy and genetics, that can rear its ugly head while training.
What is PDS exactly?
Solway says that, “PDS is notably more common in runners that have a Mortons’ type foot structure. It has nothing to do with Morton’s neuroma, which is commonly misdiagnosed for this condition. This type of foot structure will present with a longer second toe or longer second and third toes.”
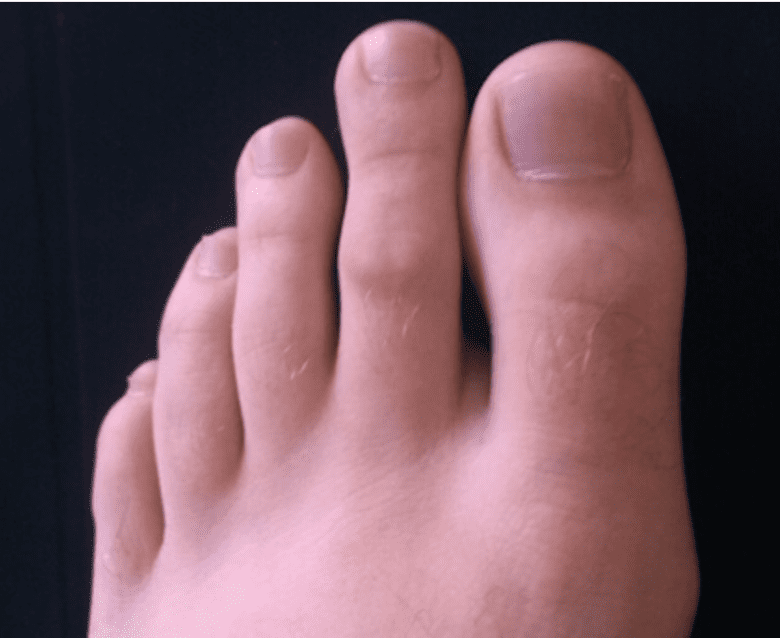
Mortons' type foot structure.
Solway continues, “This is due to the second or third metatarsals (the long bones) in your foot being longer than the average norm. Having this type of foot structure can lead to PDS over a period of time. This type of foot structure causes excessive pressure in the ball of your foot. This can cause early degenerative changes and laxity (looseness) in the soft tissue structures that stabilize the joint.”
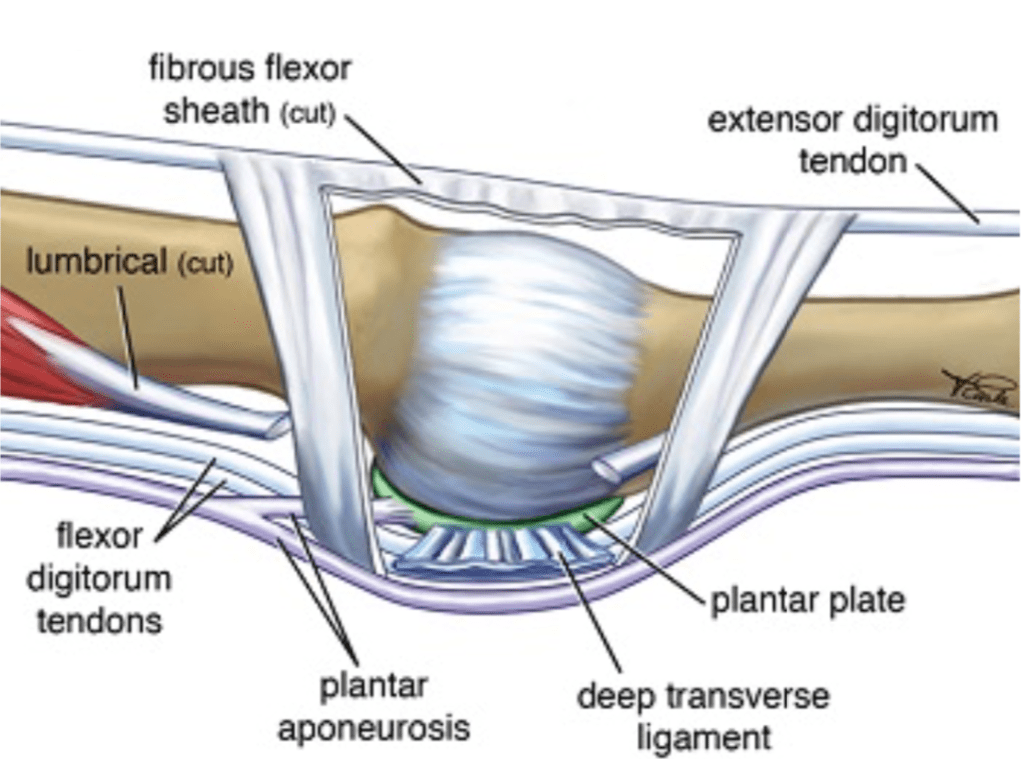
Soft tissue structures of the joint.
The symptoms of PDS can range from deep aching, burning sensations on and off the foot. There may also be a feeling of fullness or “walking on a marble” sensation. This is due to inflammation that occurs in the soft tissues surrounding the joint. PDS is a progressive condition affecting adults mostly between 45 and 75 years of age. It can also occur in younger, more active patients.
Solway says that, “This condition can eventually lead to degeneration of the soft tissue, causing subluxation (a partial dislocation) of the joint or hammering of the second and third toes, basically a contracture of the joints. This can also lead to rubbing of the toes on the shoe.”
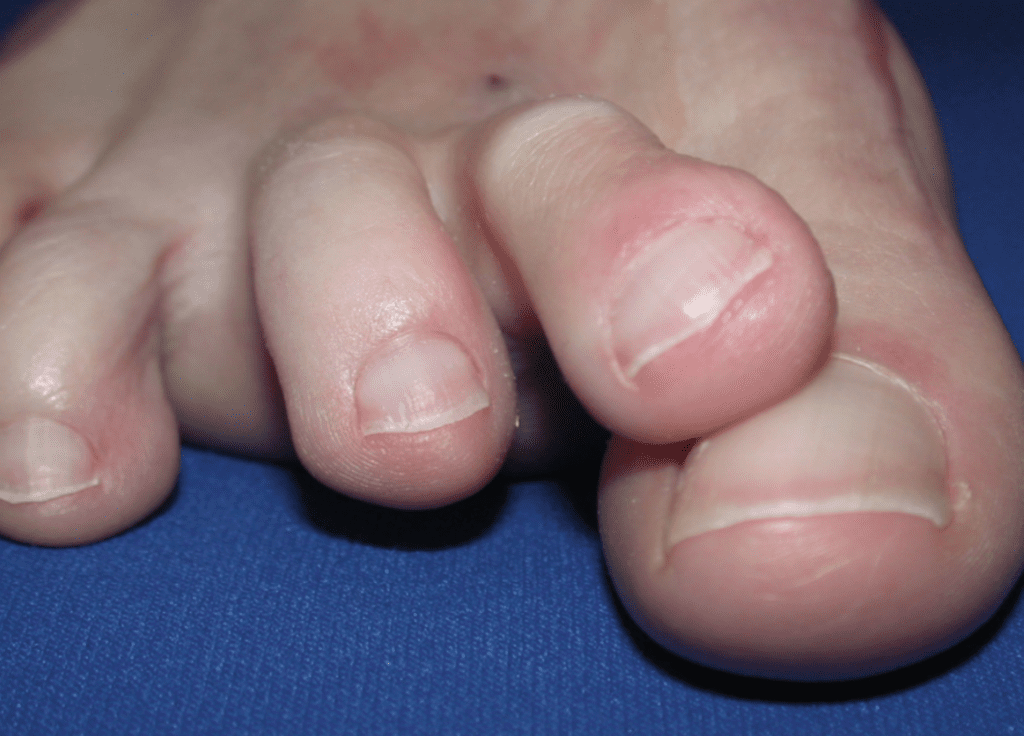
Late stage of PDS.
PDS can be easily diagnosed with an evaluation of the foot, X-ray, and sometimes an ultrasound. Causes are mostly hereditary in nature. It is based on the type of foot structure you are born with. Overuse, poor shoe gear and repetitive microtrauma can also play a part.
If caught early, PDS can be easily treated with conservative means, such as anti-inflammatories, modification of shoe gear, over-the-counter insoles and physical therapy. The goal is to reduce the inflammation as soon as possible and lend support with custom orthotics.
Although PDS is progressive, Solway says, “You can somewhat prevent its occurrence with proper running shoes, proper training, and early intervention with conservative measures. If patients continue to have pain and progression, a specially designed surgery can eventually eliminate the problem. If you feel that you have developed PDS, you should be evaluated and treated as soon as possible to slow down the process. The longer you have inflammation, the more likely you will need to have surgical correction in the future.”
You can schedule a simple screening to see if you are predisposed to PDS. If you already have PDS, remember to bring your running shoes or orthotics with to be evaluated.
Douglas Solway, DPM, is a podiatric physician who specializes in the treatment of many conditions of the foot and ankle. He offers advanced treatments such as regenerative therapy using platelet rich plasma (also known as PRP therapy), musculoskeletal ultrasound with guided injections, wound care using advanced biologics, and forefoot/rearfoot reconstructive surgery using advanced implants and new techniques.
*This content is for information only and is not intended to replace the diagnosis, treatment, or medical advice from your treating healthcare professionals. The content does not provide medical advice, does not constitute the practice of medicine or other healthcare professional services, and does not create a doctor-patient relationship. You should not rely on this information as a substitute, nor does it replace professional medical advice, diagnosis, or treatment. If you have concerns or questions, seek the advice of your healthcare professionals. If you think you may have a medical emergency, call your doctor or 911 immediately. Do not rely on electronic communications or communicate through this website for immediate, urgent medical needs. This website is not designed to facilitate medical emergencies. The use of the information is at the reader’s own risk. The links are provided for information and convenience only. We cannot accept responsibility for the sites linked or the information found here. A link does not imply an endorsement of a site.