Q&A with Dr. Rodriguez-Paez
In October of 2022, IBJI's Morton Grove DXA facility began incorporating TBS (Trabecular Bone Score), an innovative new software feature, to its bone density reports. This new diagnostic tool is rapidly becoming an important adjunct of the standard of care in the diagnosis of osteoporosis and assessment of fracture risk. It further refines our ability to provide referring physicians and their patients with the most appropriate and cost-effective care.
Read the Q&A below with Alejandra Rodriguez-Paez, MD, an IBJI board-certified rheumatologist, to learn how a bone density scan works and how TBS enhances a doctor’s ability to diagnose and treat patients.
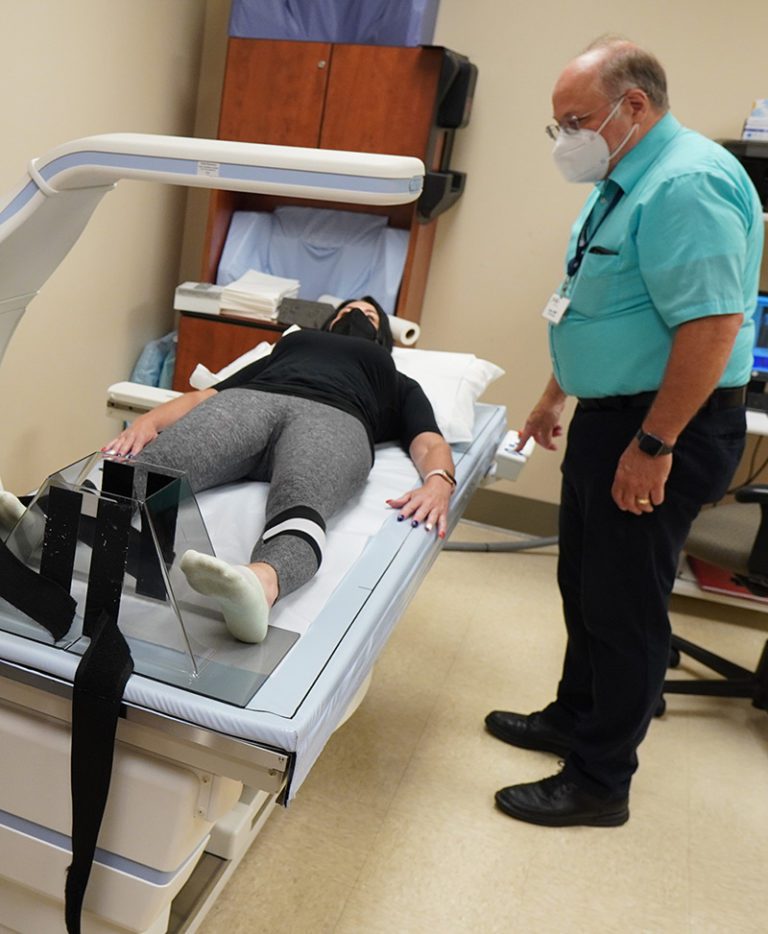
Lead DXA Technologist Larry Jankowski, CBDT, gets a patient ready for her bone
density test at IBJI's Morton Grove location.
Can you briefly describe DXA Scan? What is it?
The DXA scan is a test that measures your bone density using a technology called dual-energy X-ray absorptiometry. It is like a low-dose X-ray. The amount of radiation used in DXA is very low and less than the amount used in common X-rays and is about the same as one day’s worth of natural background radiation. This scan allows us to assess the risk of fracture (breaking a bone). We use it to diagnose bone health problems like osteoporosis.
Who is it for?
It is used in men, women, and children. It is recommended for women older than 65, men older than 70, and men and women who have risk factors for bone loss. In children, it is used for patients with a high risk for bone loss (i.e. patients with certain genetic or autoimmune disorders, taking medications that can lower bone density, such as steroids, etc).
What kind of information can be obtained from DXA scans?
It measures bone mineral density and it helps detect changes that may impact bone health. We routinely scan the lumbar spine and the hips. In certain patients, we also measure the distal forearm.
What is TBS?
It stands for trabecular bone score. It’s a software algorithm that reanalyzes DXA scan images of the spine to obtain information about the microarchitecture of the bone. It is an indirect measure of bone quality, which we could not assess before this technology existed in routine clinical practice.
Why was TBS added to our DXA scan?
Bone strength depends on the sum of two components: bone quantity and bone quality. Bone mineral density measured by DXA provides information regarding the quantity of the mineral bone only. TBS is a measurement of bone quality. Using both together gives the practitioner a better picture of the bone strength of an individual patient. This helps us assess with more accuracy the patient's risk for fracture, which leads to more precise and individualized treatment decisions.
Is this feature on all of the equipment at IBJI?
TBS was added in October 2022 and it’s only available in the Morton Grove office at this time.
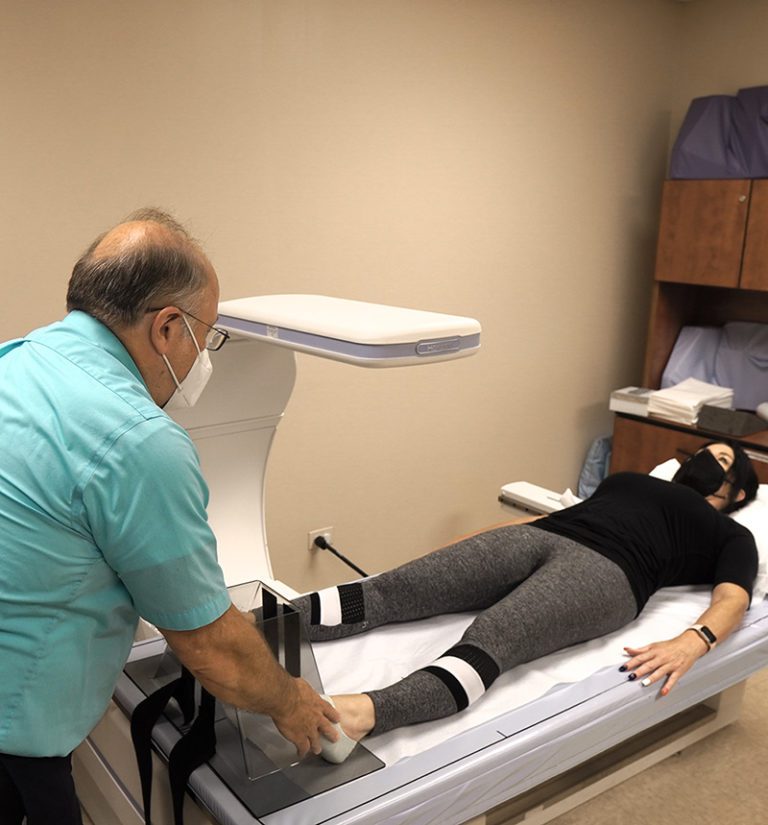
A DXA scan, combined with TBS, measures bone quantity and quality.
How does it work?
The DXA scanner takes a picture of the lumbar spine and pelvis. The TBS software is only applicable to images of the lumbar spine. The TBS software is applied to these images and calculates a score that represents the quality of its bone microarchitecture.
What does a TBS score show?
TBS has three categories: normal, partially degraded, or degraded bone microarchitecture. Higher TBS correlates with better bone microarchitecture (better bone quality) and lower TBS correlates with worse bone microarchitecture (worse bone quality).
How does knowing this score help the patient?
This information provides additional information that is additive to the bone mineral density measurement to improve our ability to decide the best course of treatment for a given patient.
Is there an extra cost associated with a DXA scan with TBS?
There is an additional cost and it is usually covered by insurance if a DXA scan is indicated for the patient. This is not a separate test. The software is applied when you have a DXA scan. It is an additional component of the DXA scan.
Does this make the DXA scan take longer than normal?
Not for the patient. A DXA scan takes about 30 minutes. However, further analysis to calculate TBS takes more time for the technician and interpreting provider.
Who shouldn’t have a DXA scan with TBS?
Certain patients cannot have a TBS. Some limitations of the test are that the TBS can only be calculated in patients where we can measure the lumbar spine. It cannot be measured in patients who have a history of extensive back surgery with hardware or other back conditions. Also, patients who are significantly obese or very thin cannot have a TBS done. It has only been validated in patients with a Body Mass Index (BMI) between 15-37.
Can you have a DXA scan with TBS if you already have osteoporosis?
Yes. It is going to be added to the routine measurement during a DXA scan in eligible patients. Unfortunately, TBS does not help in the monitoring of many of the medications used for osteoporosis.
Do you have to request TBS when scheduling your bone density scan?
No, you don’t have to specifically ask for TBS. It’s part of the standard of care available at IBJI at the Morton Grove office. This is an additional component of the DXA scan that we are using now in all patients that meet the criteria for its use.
Who performs the DXA scan with TBS?
Larry Jankowski, CBDT, is our lead DXA technologist at IBJI. He is well-known in the bone densitometry field and has published a number of articles on quality in DXA. He has trained DXA technologists around the world and currently serves as Chair of the Facility Accreditation Council for the International Society for Clinical Densitometry. All of our DXA technologists are ISCD-certified and are held to the same high standards that Mr. Jankowski has established here at IBJI.
Get more information
Visit our rheumatology page to see a list of rheumatologists who are specially trained in treating bone health disorders. You can also listen to Dr. Rodriguez-Paez’s podcasts and watch webinars on the topics of rheumatic diseases, osteoporosis, and more.
Ready to know your bone density score? Schedule a bone density scan today.